Many people ask their doctors, “How long does gout last?” In this blog, you’ll learn more about gout, including what causes it, how long flares take to resolve, complications of gout, and tips for treating gout symptoms during an acute flare. You can also understand long-term management for chronic gout by reading on.
What Causes Gout?

Hyperuricemia occurs when serum uric acid (sUA) levels are above 6.8 mg/dL. Over time, an uncontrolled, high level of uric acid can lead to the development of gout, which causes pain during acute flares and can lead to other long-term complications and health issues.
Everyone has at least some uric acid in their bodies, but too much uric acid in the blood can be problematic. Uric acid is produced when the body breaks down purines as part of normal cell replacement or by the ingestion of certain foods that have high-purine content. When there is too much for the kidneys to get rid of, it can lead to the formation of crystals in your joints and even a painful attack of gout.
Beyond elevated sUA levels, a family history of gout is the most common risk of gout.
You can reduce your risk for this painful form of arthritis by achieving a lower uric acid level through ongoing treatment and disease management.
What Does a Gout Flare Feel Like?
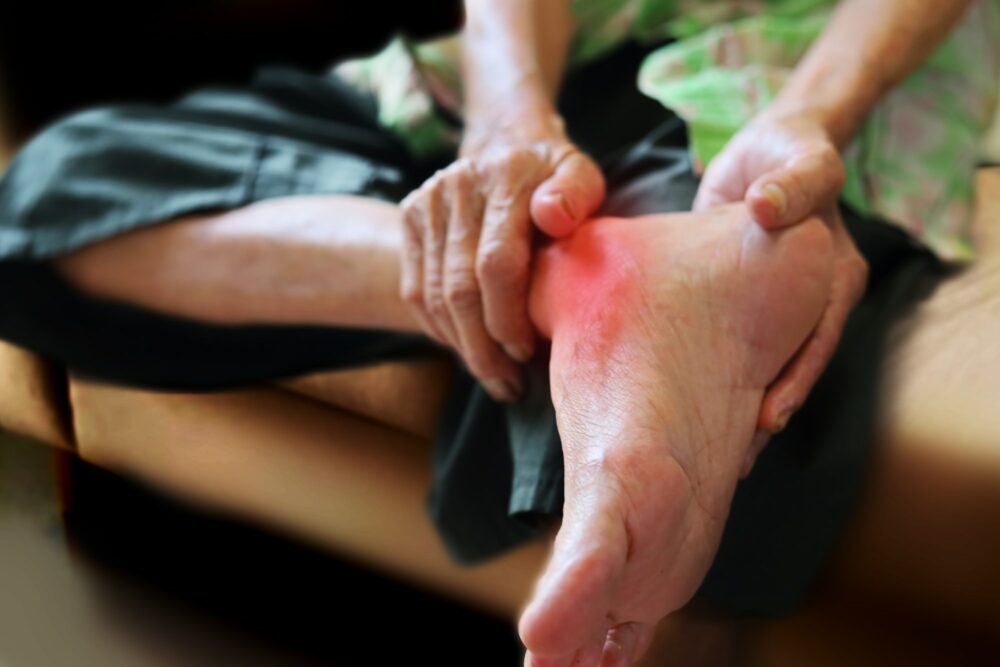
Gout symptoms include severe pain in one or more joints. The joint may be red, swollen, and very tender to the touch. People with gout usually rate the pain of gout as a nine out of 10 on a standard pain scale. Research from the Gout Education Society has found that many people would rather be hit by a car than experience the intense pain from another flare.
Gout is most common in the big toe, and severe joint pain accompanied by flares often appears there first. However, gout can also appear in other joints, such as the fingers, elbows, wrists, knees, and ankles. Over time, as crystals form in the joints, flares can become more frequent and painful if the right treatment is not in place.
How Long Does Gout Last?

Gout is a lifelong disease that must be treated and managed on an ongoing basis to keep flares under control. Still, you may be wondering how long gout pains lasts during a typical flare up. Typically, flares last three to seven days. Symptoms usually dissipate within a few days after proper treatment for joint pain and inflammation. If left untreated, a full recovery from an attack can take up to 14 days.
Untreated, gouty arthritis can lead to permanent joint damage, bone and tissue damage, and other complications, such as kidney stones or kidney disease; cardiovascular issues, such as heart attack or stroke; diabetes and more.
How Do You Treat a Flare?
Many people experiencing a flare for the first time will head to the emergency department to treat their pain. While this is okay, it is also important to follow up with a doctor after experiencing a flare so that the disease can be managed over time.
During a typical gout flare, it is helpful to keep the affected joint as still as possible and to not do anything that requires movement or adding weight or pressure to the joint until symptoms go away. If tolerated, it can be helpful to keep the joint cool with an ice pack or ice wrapped in a cloth, applying it for about 20 minutes at a time.
A gout attack usually causes severe pain, so many sufferers can’t stand it to be touched—and even a bed sheet over the affected joint can cause searing pain.
To reduce pain and swelling of an acute flare, treatment often includes anti-inflammatory medications—such as NSAIDs and/or colchicine. Corticosteroids, in the form of prednisone or Medrol, are occasionally used to treat flares when colchicine or NSAIDs cannot be used. Corticosteroids can be taken by mouth but can also be used as an injection directly into the affected joint.
A doctor (whether it’s an emergency room doctor or primary care physician) can advise on the best course of treatment to ease the pain during a flare-up. Then a rheumatologist can help with the long-term management of the disease and help reduce future flares by decreasing the level of uric acid in the body.
How Long-Term Gout Treatment Helps Beyond the Flares
After a first flare, it is important to get an official diagnosis from a doctor, typically a primary care physician. Gout can initially be mistaken for other conditions, such as sprains or strains. Conversely, many who are diagnosed with gout may have other conditions, such as pseudogout or traumatic injuries. While a blood test can measure uric acid in the body, the gold standard for making an official diagnosis is to take a sample of fluid from an affected joint as a way to detect the presence of uric acid crystals, since crystals form inside and around joints.
Lifelong treatment is typically necessary to reduce the risk of severe gout and long-term gout pain from future flares. A rheumatologist can advise on an effective treatment plan, including medication and lifestyle changes.
Medications

Once a diagnosis of gout has been made, a daily medication to reduce uric acid may be prescribed. The two most common medications, which may be used to lower uric acid in your blood and prevent future flares, are allopurinol and febuxostat. These are both xanthine oxidase inhibitors.
Like many other medications for conditions such as high blood pressure or high cholesterol, these are meant to be taken daily for life. They should not be discontinued—even when a gout flare-up is over—without first speaking with a doctor.
Without medical treatment, it is unlikely that your blood uric acid level will be lowered to the target of 6.0 mg/dL or less—a level recommended by the American College of Rheumatology—and the pain and destruction caused by flares will persist.
Diet and Lifestyle Modifications
To help prevent gout flares, many doctors will also recommend making dietary and lifestyle modifications—including making smart choices about foods and getting daily exercise.
While there is no such thing as an official “gout diet,” certain foods and diets (e.g., a diet high in purines, like red meat) have been known to trigger flares.
Some foods to avoid if you have gout may include red meat, lamb, shellfish, processed foods, alcohol (especially beer and grain liquors), sugary soft drinks and other sweetened beverages and foods. The Gout Education Society recommends limiting table sugar, table salt and products with high-fructose corn syrup to help prevent potential flares, in addition to taking daily medications as prescribed.
While there is no specific “gout diet,” many have found the Mediterranean and DASH diets to be helpful. It is also important to remain hydrated by drinking plenty of water.
More information about eating healthy with gout can be found at GoutEducation.org and through our “Gout Diet: Myth Vs. Fact” one-pager.
In addition to dietary changes, maintaining a healthy lifestyle is important. Those who have gout should talk to their doctor about a treatment plan that allows them to exercise regularly. Most adults will be encouraged to engage in moderate-intensity physical activities for at least 30 minutes most days of the week. Examples include taking a brisk walk, swimming laps, mowing the lawn, dancing or bicycling.
Always check with a physician before starting a new program or regimen.
Where to Learn More
Gout is an inflammatory arthritis caused by elevated uric acid levels, and it requires lifelong treatment and management. Knowing how long a gout flare-up lasts can help you manage symptoms, set expectations, and decide when to seek medical care. Anyone with gout can take steps to help relieve symptoms of gout flares and manage the disease for a healthier future.
More information about treatment and management can be found at GoutEducation.org.