What Is a Gout Flare?
A gout flare up, or gout attack, is typically classified as sudden and intense joint pain, swelling, inflammation and redness of a joint. A gout flare is usually warm to touch and pain is severe. Gout most commonly affects the big toe joint, but it can affect any joint at any time.
What Causes a Gout Flare?
Gout, or gouty arthritis, is a result of the buildup of urate crystals (or monosodium urate crystals) and uric acid in the blood are above 6.8 mg/dL, known as hyperuricemia. These uric acid crystals may form over years, or even decades, before a person experiences a gout attack.
When the body produces excess uric acid, it leads to a uric acid buildup and urate crystals that can develop around around joints (e.g., in the big toe, wrists, knees, etc.) and other tissues.
When there is more uric acid than the kidneys can get rid of, the build-up can lead to a gout attack. If this is not addressed in a timely fashion, a future gout flare-up is possible, leading to joint destruction and chronic arthritis (sometimes referred to as chronic gout, however, all gout is considered chronic).
Over time, this condition can wreak havoc on the body contributing to other serious health issues. Proper and timely disease control is important.
Risk Factors of Flares
The biggest risk factor for a gout flare is excess uric acid levels above 6.8 mg/dL. Those who have gout should aim for below 6.0 mg/dL to avoid future flares.
Beyond this, gout is also connected to several risk factors, including family history; obesity; poor dietary or lifestyle choices; use of certain medications (e.g., diuretics or beta-blockers); and other health issues. When gout is not properly treated, uric acid crystals can continue to build around and deposit in the kidneys—ultimately leading to kidney stones and even chronic kidney disease.
Other serious health issues that have been connected with incident gout include heart attack, heart disease and stroke, as well as diabetes.
Symptoms of a Gout Flare
Common symptoms of a gout flare up include the sudden onset of severe pain, swelling, redness, and tenderness in the affected joint.
Upon physical examination, a gout flare in an affected joint may look like this:
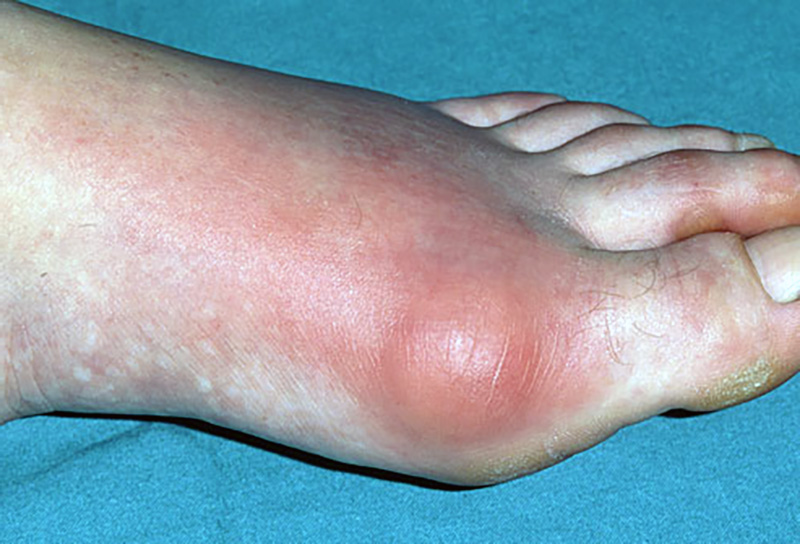
There is a common misconception that clinical manifestations of gout will appear in only one joint at a time, especially in the big toe joints. This is untrue, as gout pain can present itself in several parts of the body at a time. If you are experiencing a flare in one joint, you can’t rule out the potential of gout affecting other joints.
Pain
Gout is so excruciating that most people rate their pain level as 9 out of 10. Even a bed sheet touching the big toe—or other toe joints if affected—in the middle of the night can lead to extreme agony.
Acute attacks can last from five to ten days without proper treatment and can result in debilitating pain.
According to a study conducted on behalf of the Gout Education Society, half of people with gout say that they cannot imagine anything more painful than a gout attack.

Furthermore, symptoms of gout attacks can put tremendous emotional burden on a person, on top of the physical pain they are experiencing. For example, the study found that one in four people with gout frequently misses work because of gout—and more than half of people with gout are embarrassed that they have it.
Gout Attack Triggers
Painful gout flares are triggered when too much uric acid builds up and crystals accumulate and affect one or more joints. The below list includes some of the more common triggers, however, it’s important to note that triggers may be different for everyone. For more information, check out our Gout Flare Triggers page.
Alcohol Consumption
Excessive intake of alcohol, particularly beer and grain alcohol, is a trigger that is commonly reported by people with gout because it can lead to elevated levels of uric acid. When it comes to alcohol consumption, moderation (paired with keeping uric acid levels low) is key to managing flares.
Purines and High-Fructose Corn Syrup
A diet rich in purines—which can be found in foods like red meat, shellfish, and organ meats—can trigger flares by increasing levels of uric acid in your body. It’s also important to avoid foods with high-fructose corn syrup, such as soft drinks, sweetened fruit juices, sugary cereals, ice cream, and most processed foods. Again, moderation is key. When uric acid is under control, those who have gout should be able to enjoy treats!

Crash Diets
It’s important to get professional medical advice before making any major dietary changes. “Fad” diets, like those based around high protein/purine-rich foods (e.g., red meat), can take a toll on the body. While losing weight can be helpful to lower the risk of gout, it’s important to do so in a healthy manner.
Surgery, Trauma or Sudden Illness
Those who are immobile for long periods of time (like after surgery or while sick) are at higher risk for gout flares.
Starting Uric Acid-Lowering Medicines
While this may seem counterproductive, starting a uric acid-lowering medication can actually trigger flares. This is because the body is working hard to eliminate the excess uric acid and lower uric acid levels. A period of increased risk of flares only lasts for about three months after starting the uric acid-lowering therapy, and your doctor should be giving anti-inflammatory therapies during this period to lessen the risk.
Even if flares are experienced, it’s important to stick to professional medical advice and take medications as prescribed. Talk to your doctor before suddenly stopping or starting medications.
Treatments for Gout Flare-Ups
It’s important to begin taking your prescribed gout medication as soon as possible to resolve current symptoms and avoid future flare-ups.
It’s important to keep your medications on you at all times, especially if you’re traveling. If you do not have them on hand, call your doctor and ask for a prescription to be filled at the nearest pharmacy.

Pain Management
There is no one-stop-shop treatment to stop a gout attack once it has started. The primary goal is to manage the pain associated with the symptoms of a flare-up. There are certain medications often prescribed by medical professionals to eliminate pain and inflammation. All of the approaches mentioned below are equally effective but need to be started within the first half-day of gout flare symptoms.
Colchicine
This is the most common treatment prescribed for those experiencing a gout flare. Colchicine is most effective if taken within the first 12 hours of experiencing symptoms. A common timeline for taking low doses of colchicine at the onset of a flare is to take two tablets (0.6 mg per tablet) at once, then a third tablet one hour later, followed by one tablet one to two times per day over the next week.
Nonsteroidal anti-inflammatory drugs (NSAIDs)
Most over-the-counter NSAIDs, like Advil®, Aleve®, and Motrin®, are readily available at your local drug store and can relieve pain effectively. If the standard doses do not work for you, your doctor may prescribe high doses of prescription versions of nonsteroidal anti-inflammatory drugs, like Celebrex®, Indocin®, or Naprosyn®.
Glucocorticosteroids
Used to suppress the inflammation of acute attacks, these can be taken orally or injected. Glucocorticosteroids work quickly and might be prescribed under brand names, like Deltasone® (prednisone), Kenalog®-40, or Medrol®.
Other Treatments
Aspirin is commonly thought of as a quick management medication, however, it should not be taken during a flare. The only time this is an acceptable treatment is when low-dose aspirin has been prescribed by a medical professional for heart disease prevention.
Gout Flare Up Prevention
Once one gout flare up has occurred, it’s likely that another will happen at some point. Recurrent gout, or chronic gout, is likely to be diagnosed over time. While it’s almost impossible to predict when the next will happen, there are steps to take to decrease the risk of a flare and future bone, tissue, and joint damage.
Keep Uric Acid Low
If your body produces too much uric acid, you’ll always be on the verge of gout symptoms. It’s important to stay on your prescribed urate-lowering medication. By keeping your uric acid levels low (below 6.0 mg/dL), you can reduce the chance of flares and the overall burden of gout.
Avoid Triggers
Gout affects everyone differently, especially when it comes to flare triggers and gout symptoms. It’s important to recognize what triggers lead to flare-ups. Recognizing these triggers can help you avoid increased risk for flares and even make changes, like switching to a healthy diet or exercising regularly, to manage gout and other chronic conditions better.
Keep Track of Flares
Self-management is a key method of reducing the potential of recurrent gout attacks. Understanding and keeping track of your gout symptoms can help you have more meaningful conversations with your doctor and lead to better treatment overall.
We have created a scorecard to help gout patients keep track of flares and other healthy benchmarks to reduce the risk of gout flares. Other benchmarks to watch out for include high blood pressure, cholesterol levels, blood sugar, and more.
Talk to Your Doctor
If self-management is not helping your gout—or you’re not happy with your current treatment regimen—it may be time to find more specialized care.
Rheumatologists, who are often known for treating chronic arthritis, rheumatoid arthritis, are the go-to specialists for treating gout.
To help you in your search for optimal care, we’ve created the Gout Specialists Network. Take a quick survey to find a doctor near you.
To learn more, check out our other resources.